LongevityWay Weekly
Hey Longevity freaks. Quick, evidence-first hits — minus the hype.
Today’s lead: longevity science just took a step from “interesting in mice” to “show me in humans.” A federally funded U.S. program is now putting real money behind testing whether existing drugs can preserve function and extend healthspan — not just treat one disease at a time.
What’s inside this week
🧪 Big Story: A $38M national trial will test drugs to extend healthspan
🧠 News: Annovis’ Alzheimer’s drug moves forward — but the real proof is still ahead
🚶 Practical science: Tiny lifestyle changes still punch above their weight
⌚ Biohacker Arsenal: Step counters — the lowest-friction longevity tool
💊 Supplement of the Week: Omega-3 (EPA/DHA)
👤 Person to Follow: Dr Elena Volpi
LATEST NEWS
LATEST NEWS
🧪 A $38 Million U.S. Trial Will Test Whether Existing Drugs Can Extend Healthspan
The Summary
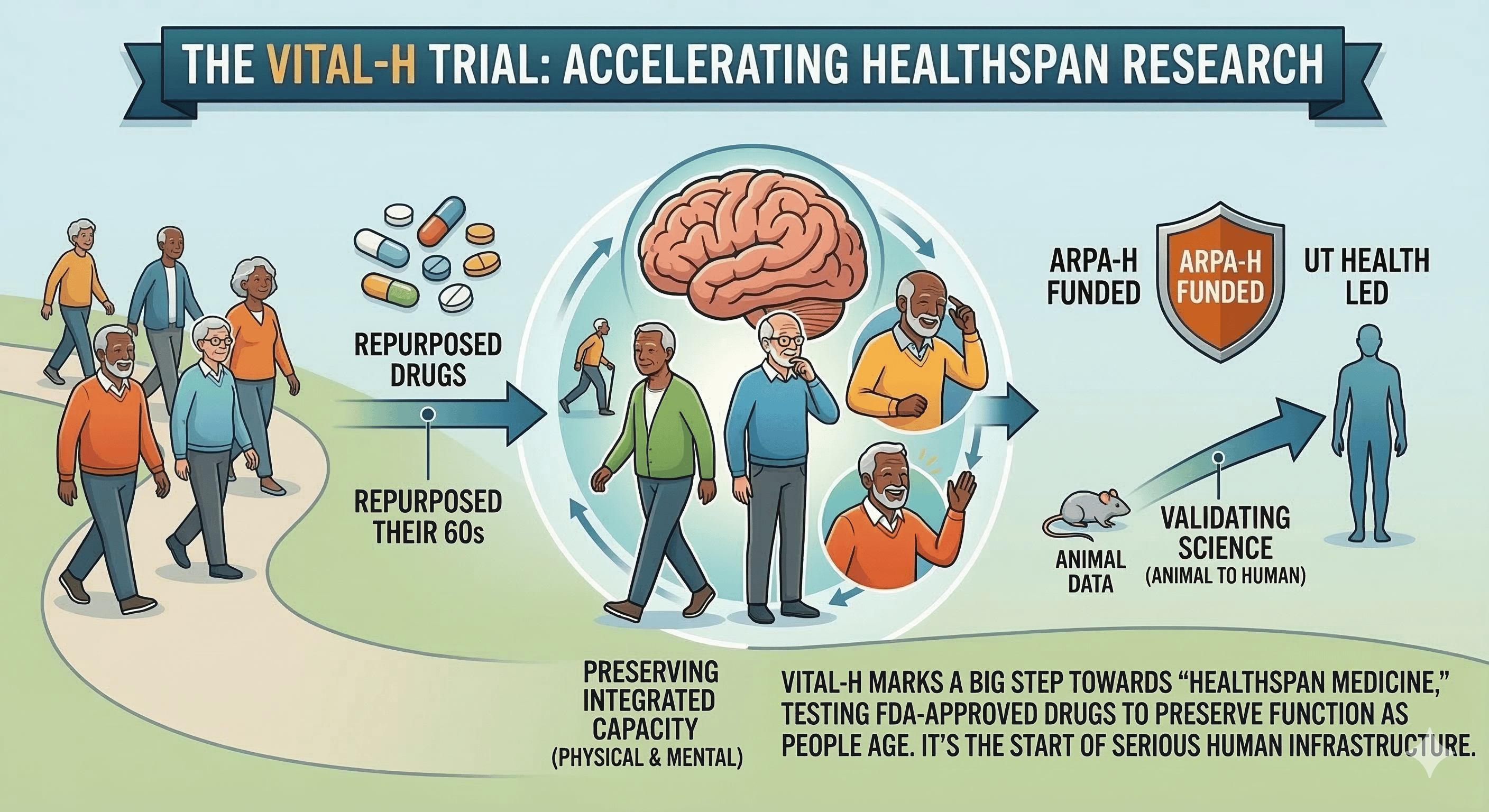
UT Health San Antonio is leading a five-year, ARPA-H-funded trial called VITAL-H that will test whether rapamycin, dapagliflozin, or semaglutide can help preserve health and function as people age. It’s one of the clearest signs yet that longevity research is moving into large-scale human testing.
Key Details
Funded for up to $38 million through ARPA-H’s PROSPR program, which is focused on extending healthspan.
Planned enrollment is 726 adults in their 60s, split across four arms: rapamycin, dapagliflozin, semaglutide, and placebo.
Participant enrollment is expected to begin next year.
The trial is also testing whether intrinsic capacity — a combined measure of physical and mental function — can work as a serious endpoint for healthy-aging trials.
The big signal here is not “these drugs work already,” but that regulators and mainstream institutions are now treating healthspan as something worth measuring in humans.Practical takeaway
Why It Matters
Longevity research has had plenty of promising animal data. What it has lacked is serious human infrastructure. VITAL-H is one of the strongest signs yet that healthspan medicine is trying to grow up.
LATEST NEWS
🧠 Annovis’ Alzheimer’s Program Moves Forward — But Don’t Call It a Breakthrough Yet

The Summary
Recent coverage highlighted Annovis Bio CEO Maria Maccecchini saying the company expects an important milestone for its Alzheimer’s program in March or April. The official update behind that attention is that an independent Data and Safety Monitoring Board found no safety concerns at 6 months, allowing the pivotal Phase 3 trial of buntanetap to continue.
Key Details
The Phase 3 Alzheimer’s study is currently recruiting in the U.S. and Annovis says it is about 40% complete.
The company says the first symptomatic efficacy readout is expected in early 2027.
A disease-modifying readout is expected in early 2028.
Annovis also announced upcoming presentations at AD/PD 2026 covering Parkinson’s data and updates from the Alzheimer’s program.
For longevity readers, the main relevance is obvious: anything that genuinely protects brain function would matter hugely for healthspan, but this is still a watch-the-data story, not a confirmed breakthrough.
Why It Matters
Anything that genuinely slows neurodegeneration would be huge for healthspan. But Alzheimer’s drug development is where hype goes to get humbled, so the standard here has to stay brutal: show the actual clinical benefit.
LATEST NEWS
🚶 Tiny Lifestyle Tweaks Still Matter More Than Most Biohacks

The Summary
This week brought fresh coverage of a very useful message: small, realistic changes still compound. The underlying University of Sydney research was published earlier this year, but it remains one of the most practical healthspan findings around.
Key Details
In nearly 60,000 UK Biobank participants, researchers found that among people with poor baseline habits, adding about 5 minutes of sleep, 2 minutes of moderate-to-vigorous activity, and half a serving of vegetables per day was associated with roughly one extra year of life.
Stronger combined improvements were associated with more than 9 extra years of lifespan and healthspan.
A second study from the same release found that 5 extra minutes of moderate-paced walking/activity per day was associated with about a 10% lower chance of early death.
Cutting 30 minutes of sedentary time per day was linked to about a 7% reduction in all-cause mortality.
The useful takeaway is simple: for most people, you do not need a perfect routine — slightly better, done consistently, can matter a lot.
Why It Matters
Longevity content often fails because it makes people feel they need a new identity. This line of research says the opposite: micro-wins compound. That’s a message normal humans can actually use.
BIOHACKER GADGET COMPARISON
⌚ Step Counters: the easiest longevity tool you’ll actually use
The Summary
If you want one cheap, low-friction tool that makes “move more” real, it’s a step counter. Not because steps are magic — but because they turn vague advice into a number you can actually improve.
Key Details
A 2025 systematic review and dose-response meta-analysis covering 57 studies from 35 cohorts found that daily steps were linked to a wide range of outcomes, including all-cause mortality, cardiovascular disease, type 2 diabetes, dementia, depressive symptoms, and falls. For several outcomes, the curve started bending meaningfully around 5,000–7,000 steps/day. Compared with 2,000 steps/day, 7,000 steps/day was associated with 47% lower all-cause mortality, 47% lower cardiovascular mortality, 38% lower dementia risk, and 22% lower depressive symptoms.
Pick one
Phone step counter if you want zero extra cost
Basic pedometer if you want simple, no distractions
Watch/band if you also want sleep and heart-rate trends
The best one is the one you’ll actually keep using.
Big caveat
Steps are not the whole game. You still need strength training, decent sleep, and basic nutrition. And the step data are still mostly observational. But as a behavior-change tool, this one is hard to beat.
SUPPLEMENT OF THE WEEK
Creatine Monohydrate — cheap, boring, and surprisingly useful
The summary
Omega-3 is not a miracle longevity pill. But it is one of the more evidence-backed basics for cardiometabolic health, especially if your intake is low or your triglycerides are high. According to the NIH Office of Dietary Supplements, fish oil and other long-chain omega-3 supplements lower triglycerides and might reduce some cardiovascular endpoints, with stronger evidence in higher-risk groups than in healthy low-risk people.
Benefits:
Triglycerides: clearly lowered, especially at higher doses and in people with higher baseline levels.
Cardiovascular risk: some evidence of reduced cardiovascular mortality/coronary outcomes, but results are mixed and not all endpoints improve.
Pick this:
✅ Choose an omega-3 that clearly shows the actual EPA + DHA per serving, not just “fish oil 1000 mg.”
✅ Choose a product with around 500–1000 mg combined EPA + DHA per daily serving as a solid general-use default.
✅ Choose fish oil as the best default for most people, or algal oil if you want a vegetarian/vegan option.
❌ Avoid products that only show total fish oil but hide the actual EPA and DHA amounts.
❌ Avoid choosing based on “wild salmon” branding alone, because EPA/DHA content and quality control matter more.
❌ Avoid overpaying for krill oil if the EPA/DHA dose is lower and the price is higher.
Safety (when to avoid / be careful)
The AHA does not recommend omega-3 supplements for everyone at low cardiovascular risk, and high-dose omega-3s have been linked in some trials to a slight increase in atrial fibrillation risk in people with cardiovascular disease or high risk.
PERSON TO FOLLOW
Dr Nir Barzilai — @NirBarzilaiMDAbout
He’s one of the most important names in human longevity research, especially around centenarians, longevity genes, and gerotherapeutics, and his X handle is @NirBarzilaiMD.
1
